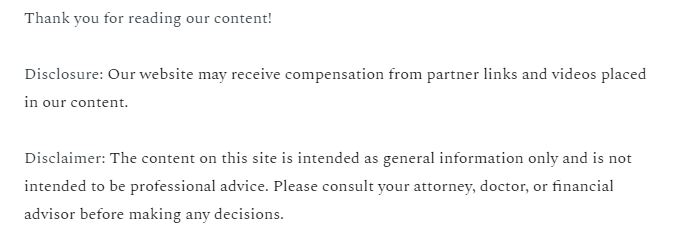
In South Africa, many pregnant women and girls are avoiding testing at prenatal clinics — not for pregnancy but for HIV. The problem stems from many of the clinics’ practices, which could be contributing to the high mortality rate of pregnant women in the region.
Although prenatal care is available for free under South Africa’s public healthcare system, Amnesty International reports that these young women are avoiding their local clinics because of practices that could intentionally reveal their HIV status to other patients.
In addition to giving pregnancy tests, clinics will also often test for HIV. Many of these women already know their status, but the clinics do not always practice strict patient confidentiality when their patients are present.
Amnesty International visited with pregnant women in the provinces of Mpumalanga and KwaZulu-Natal, and they compiled their research in their report Struggle for Maternal Health: Barriers to Antenatal Care in South Africa.
The findings were not only problematic but deadly, as well. One woman from KwaZulu-Natal said that the clinic nurses would openly talk about patients and their HIV status.
In general, the clinics used non-verbal methods that would disclose the status of their patients. Some held separate lines for antiretroviral medications; others would store information in different colored files for HIV positive and negative patients, and some would even schedule HIV positive patients’ appointments on separate days.
One woman in Mpumalanga explained that “If women come out of the counselor’s room with two files, then everyone knows they are HIV positive.”
Women in these communities face significant HIV-related stigma, including discriminatory treatments from partners and family members if they are exposed as HIV positive.
The reports findings are grim when coupled with what Amnesty International refers to as an “unacceptably high rate of maternal mortality.” In 2011, the country recorded 1,560 maternal deaths; in 2012, the number dropped only slightly to 1,426.
Further, more than one-third of those deaths were linked to HIV, but health experts estimate that 60% of all maternal deaths in those years were avoidable.
“While HIV testing is an important public health intervention it must be done in a manner that respects the rights of women and girls and does not expose them to additional harm,” said Salil Shetty, Amnesty International’s Secretary General. “It is deeply worrying that the privacy of pregnant woman and girls is not respected in health facilities.”
Shetty also commented that it is up to the South African government to intervene and correct the issue. The country also has a number of issues with infrastructure, as even emergency vehicles cannot drive on certain roads during rainy weather.
In addition to mortality rates, the report also identified a lack of information available for women about sexual and reproductive health. As a result, women, especially adolescents, are at increased risk for unplanned pregnancy and HIV transmission, and they are also often unaware of the importance of prenatal care.
“Being tested for HIV during pregnancy is vitally important for the wellbeing of the unborn child,” says Carla Sebaski, RN, Nurse Manager at CareNet Pregnancy Services of DuPage. “If HIV positive and left untreated, there is a 1 in 4 chance of infecting your baby. However, if the mother takes the appropriate prevention measures, that risk drops as low as 1 in 100.”
Overall, the report urged the country to protect the confidentiality of patients, improve knowledge of sexual and reproductive health and rights for men and women, increase the access to care for girls and women through means such as public transportation, and improve the country’s infrastructure so emergency vehicles can travel on all roads.